Premenstrual Syndrome is an extremely fascinating aspect of Wilson’s Temperature Syndrome. In may ways, the symptoms of Premenstrual Syndrome (PMS), are remarkably similar to the symptoms of DTSF and may include lightheadedness, dizziness, gas bloating, weight gain, fluid retention, headache, depression, irritability, fatigue, constipation, increased bruising, muscular aches, and others. It is also well known that PMS symptoms follow a menstrual pattern, typically being more severe right before a woman’s menstrual cycle begins. However, I have seen some cases where the patients’ symptoms are aggravated just after their period with their symptoms being exactly like the symptoms of PMS except happening “post”-menstrual. So there are some people who have PMS after their period or-“Postmenstrual Syndrome.” This can easily be explained within the framework of Wilson’s Temperature Syndrome. It is well known that a woman’s body temperature will change during her menstrual cycle, commonly spiking (rising sharply) at ovulation and often averaging highest prior to or at the beginning of a woman’s period. The temperature typically will decrease gradually during the menses and may even reach a low point after the period is over.
As discussed previously, the symptoms of Wilson’s Temperature Syndrome are preeminently symptoms of Multiple Enzyme Dysfunction that are caused by aberrations in enzyme temperature. Temperature changes that can affect enzyme function can include temperatures that are too low, too high, or too unsteady. Rapidly changing body temperatures can cause enzyme dysfunction because of a too rapid change of enzyme shape/configuration that does not allow proper enzyme function. Premenstrual symptoms can easily be explained by enzyme dysfunction brought on by abnormal body temperature patterns (too low, too high, or especially unsteady/changing rapidly). This can also explain why some women have similar symptoms at the time of ovulation (there are still those who do not believe that some women who can tell fairly well when they ovulate), and post menstrually. Women trying to get pregnant will frequently take advantage of these well known menstrual cycle related body temperature changes by taking daily temperatures, in an attempt to identify the time of ovulation by the mid-cycle body temperature “spike”.
Incidentally, this can explain what one might call “reverse PMS.” There are patients who will feel the symptoms of MED, being tired, depressed, bloated, irritable, etc. for most of the month, but notice that just prior to their menstrual cycle, they may enjoy two days out of the month when they feel much improved before feeling worse again. It may be that the patients’ MED symptoms are resulting from persistently low body temperature patterns that improve briefly just prior to the period as the female hormone system raises the body temperature. This causes the patients’ body temperature patterns to more closely approach normal for a brief period of time, helping them to enjoy improvement in their symptoms of MED. When patient’s symptoms of MED come and go giving them good days and bad days, patients can frequently see that their body temperature patterns are closer to normal on their good days as compared to their bad days.
Of course, menstrual cycles are female hormone related. And certainly, body temperature patterns change in a predictable and reproducible way during the menstrual cycle. It stands to reason, therefore, that female hormones may have an influence on body temperature patterns. Thyroid hormones also affect body temperature patterns, and body temperature patterns correlate well with symptoms of MED. So it follows that body temperature patterns depend, to a degree, on the relative influences of the female thyroid system (a
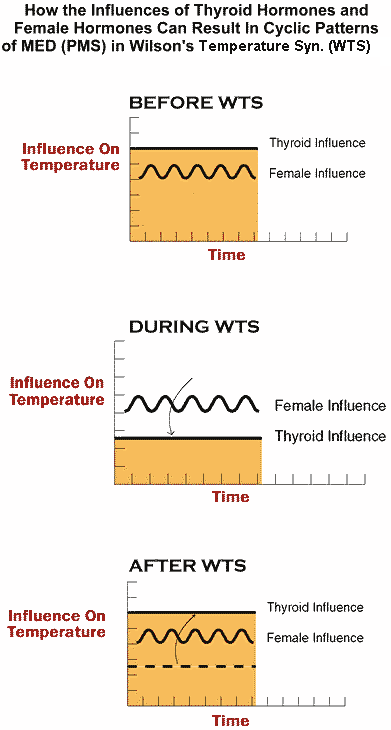
cyclic influence) and the thyroid system (a more constant influence). It seems that the more steady thyroid hormone influence on body temperature pattern, normally dilutes the more cyclic influence of the female hormone system, preventing the body temperature pattern from being so aberrant that it result in the symptoms of MED. However, when the thyroid system influence decreases because of Wilson’s Temperature Syndrome, more of the cyclic influence of the female hormone system can be “unmarked” leading to symptoms of MED that can worsen and improve in a pattern that correlates with the menstrual cycle (Premenstrual Syndrome).
When PMS is caused by Wilson’s Temperature Syndrome, the MED symptoms that seem to follow a female hormone influence can often be completely resolved with the WT3 protocol. By restoring the more stabilizing influence of the thyroid system to normal levels, one may dilute the cyclic influence of the female hormone system once again (“masking” it), thereby, eliminating the symptoms of PMS. (See following diagram)
This explains why female hormone therapy can sometimes be used to improve the symptoms of PMS (by altering the female hormone influence). It is difficult, however, to diminish the cyclic influence of the female hormone influence using female hormones because it is difficult to predict when that influence is on the way up and when it is on the way down. If the female hormones are added at the wrong time, the additional influence may add on to a “peak” rather than filling in a “valley” which can make the situation worse.
For this reason, female hormones frequently fail to eliminate the symptoms of PMS completely. And the PMS symptoms do not commonly remain persistently improved after female hormone therapy has been discontinued. This suggests that the female hormone therapy may not be addressing the underlying problem.
I sometimes use the following analogy to explain the use of female hormones and thyroid hormones in addressing the problem of PMS: If you needed something that was on a shelf that was too high to reach, you could either lower the shelf or get a stepladder (two solutions to the same problem). In that same way, both thyroid and female hormones can be used to affect the symptoms of Premenstrual Syndrome. The most appropriate treatment depends on the underlying cause of the symptoms. If the symptoms of PMS appear in combination with other symptoms of Wilson’s Temperature Syndrome and they appear in a group, especially worsening after a major stress, then it is more likely that all the symptoms are related, and it is more likely that they are related to an impairment in the conversion of T4 to T3 resulting in aberrant body temperature patterns. Patients with Premenstrual Syndrome related to Wilson’s Temperature Syndrome often find that when they are properly treated with liothyronine, that their symptoms can be alleviated greatly and often completely. Again, when careful history is taken, one may find that a patients’ PMS symptoms appeared initially or became especially worse after a major stress such as childbirth or divorce. I have treated many patients who have continued to be troubled by severe and even disabling PMS in spite of having received other treatments for years. Many times with proper T3 treatment normalizing their body temperature pattern, the patients will find that for the first time in years their period can sneak up on them (and their clothes) without the first PMS symptom or warning. Needless to say, these patients and their families are quite happy when the PMS resolves.