Wilson’s Temperature Syndrome is the cluster of often debilitating symptoms especially brought on by physical or emotional stress that can persist even after the stress has passed (due to maladaptive slowing of the metabolism), which responds characteristically to the normalization of body temperature patterns (especially through the use of the WT3 protocol defined in the Doctor’s Manual for Wilson’s Syndrome). It is characterized by a body temperature that runs, on average, below normal, and routine thyroid blood tests are often in the “normal” range.
Now, let’s go step-by-step through the definition so that we can more fully characterize Wilson’s Temperature Syndrome.
A Cluster Of Seemingly Unrelated Symptoms
A cluster, because the symptoms tend to come on together in a group. All of us, when asked to describe what it feels like to have a fever, can give extremely similar answers, since elevated body temperature patterns can cause characteristic complaints. So, also, can low body temperature patterns cause characteristic complaints.
Since the body temperature is so fundamentally important in many of the processes of the human body, an abnormally low body temperature pattern can cause a multitude of different symptoms. Usually, but not always, patients suffering from Wilson’s Temperature Syndrome complain of many of the symptoms (rather than just a few). Although they can come and go separately at different times, they frequently come on together in a group also. When the symptoms come and go together at the same time under the same circumstances, it is more likely that they are related.
It is extremely interesting that the symptoms don’t always follow the same order of severity in every patient. For example, when I am interviewing patients I will always ask them which symptom or complaint is bothering them the most. Sometimes it will be fatigue, sometimes depression, sometimes migraines, sometimes PMS, sometimes fluid retention, etc., etc. In fact, almost every one of the symptoms listed in this book has been claimed by one patient or another as being their most significant complaint. So one can see how varied the presentation of Wilson’s Temperature Syndrome can be.
Some of the symptoms can seem unrelated because it is hard for most people to understand how one problem can be the cause of so many different complaints. But when one understands the fundamental importance of body temperature patterns on the functioning of the human body, it becomes much less difficult to understand.
As we have discussed, body temperature patterns reflect the thyroid hormone/thyroid hormone receptors interaction and closely correlate with the resulting symptoms of decreased thyroid system function. So any thyroid hormone treatment that does not consider body temperature patterns may not adequately alleviate the resulting symptoms of DTSF. The treatment described in this book does take into consideration the body temperature pattern, as well as peripheral conversion of T4 to T3. Since this treatment more effectively addresses the underlying problem and is directed towards the root of the problem, it more effectively alleviates the symptoms of DTSF when they are present, improving the symptoms both more completely and more quickly. Because of this, it is more evident which symptoms improve together, and therefore, which symptoms are more likely to be related. It becomes apparent that there are many more symptoms related to DTSF than has been previously realized.
What is interesting is that these symptoms appear not to be just a little related, but very much related to DTSF. For example, dry coarse skin, impaired memory, constipation, hair loss, brittle nails, depression, and fluid retention are well known symptoms related to hypothyroidism. But other symptoms, generally not considered as being related, including panic attacks, premenstrual syndrome, migraine headaches, irritability, asthma, allergies, and others, have been found to be.
Brought On By Stress
The symptoms usually come on together, especially after significant physical, mental, or emotional stress. The symptoms cannot always be easily related to episodes of stress, because sometimes the onset of symptoms is more subtle. But when they come on together after a significant stress, they are easier to recognize as being related. As has been pointed out earlier, the body frequently responds to stress by slowing down the metabolism, by slowing down the conversion of T4 to T3. It does this to conserve energy. The only problem is that the impaired conversion of T4 to T3 can persist even after the stress has passed, causing a person to be inappropriately stuck in the conservation mode. This can prevent him/her from being as productive as s/he otherwise might be and may lead to inappropriately persistent symptoms.
If careful histories are taken, one may find that patients will go through a period of stress and will slow down. When the stress is over, they will usually come back up to normal. Later they may slow down and come back up to normal after another stress. Then finally, after one particular stress, a patient may slow down, develop symptoms of Wilson’s Temperature Syndrome, and stay down even after the stress resolves. Subsequent stresses may further impair the patient’s conversion of T4 to T3, and some of their persistent symptoms may worsen and they may also develop additional symptoms.
So really Wilson’s Temperature Syndrome is a coping mechanism gone amuck, an adaptive response responding maladaptively. It is a condition that can persist for many, many years, even forty to fifty years. It is not an immediately life-threatening condition, but it may contribute to increased deaths over time from higher cholesterol levels and coronary artery disease. And it can affect, to an amazing degree, the quality of life and productivity of a person. But, if recognized and properly treated, it can often be easily remedied.
However, subsequent stresses can cause this problem to return. Typical episodes that can precipitate the symptoms of Wilson’s Temperature Syndrome include childbirth, divorce, death of a loved one, job or family stress, surgery or accidents, smoking and then quitting, and others. It is quite common for patients to pinpoint the fact that after a certain stressful event in their life such as the death of their father, they identifiably, and unequivocally have not been the same since (even though it may have occurred fifteen or twenty years previously). Sometimes they attribute the way they feel to the loss being so great, they sometimes feel that it changed the whole condition of their lives. However, for some patients, even though their father did die, they feel they have bounced back fairly readily (being left without financial problems and still having plenty of loved ones and family members to whom they can relate), but they still cannot seem to return to normal. The patients themselves will often be perplexed as to why they should stay persistently symptomatic and never quite get over the traumatic experience, even though mentally and psychologically they feel that they have recovered. They may have been close to their father, but they know that their father would have them get on with their lives and they feel fully psychologically and mentally prepared to do it, but they still have significant physical problems which they cannot overcome. These patients frequently get their answer when they come to realize that their physical complaints and problems weren’t psychological, or mental at all; when with proper thyroid hormone therapy their symptoms resolve with normalization of body temperature patterns and the restoration of their metabolism back to the productivity mode.
The Patient’s Story
1. When patients with Wilson’s Temperature Syndrome go to a doctor for relief, it is helpful to determine what complaint is bothering the patient the most. This is what is known as a chief complaint. Sometimes patients will offer only a chief complaint without volunteering any other symptoms. This may be because they don’t realize that their other symptoms could possibly be related, or because they are not of a severity that concerns the patient, or perhaps because they are afraid to be labeled complainers or hypochondriacs. But, additional complaints, or characteristics can provide important clues to the underlying ailment or condition.
2. It is also helpful to ascertain from the patient when the major complaint or complaints first began. Wilson’s Temperature Syndrome is more obvious when the complaints come on together in a group after a major stress because the onset is more identifiable. However, some patients have more subtle presentations, having some of the symptoms for even all of their lives. Frequently, the symptoms will worsen after subsequent stresses becoming progressively worse and more pronounced, and may even increase in number. It is also helpful to inquire of the patient what situations or circumstances seem to make the symptoms worse and which seem to make them better. Patients may notice that under conditions in which they are not under as much stress, when they are able to get more regular exercise, and with certain eating habits such as a hypoglycemic diet (for example, higher in protein, lower in carbohydrates taken in six small meals rather than in three large meals per day), their symptoms will often improve greatly.
3. It is also helpful to find out from the patient if these symptoms have responded to treatment of any kind in the past, and if the patient has been treated previously with thyroid medication. The symptoms of Wilson’s Temperature Syndrome often improve in a group when patients are given thyroid medication. However, when a patient with Wilson’s Temperature Syndrome is treated with thyroxin (T4), the symptoms usually improve for a period of time (usually for about three months), and then will often go downhill again. If the dose of thyroxin is increased the patient’s symptoms will, again, frequently improve for a short period of time (often the same amount of time as with the first dosage), with the symptoms then worsening again. This cycle may repeat itself several times, with the patient’s symptoms improving for a time and then worsening again with each successive increase of T4 medication. Frequently, if the T4 dosage is increased one too many times, then the symptoms can worsen “right off the bat” without there first being any improvement. This is generally an unfavorable sign that indicates that the patient’s thyroid system is being pushed too far in the wrong direction, with the wrong medicine, because of the feeding of the vicious cycle of T4 to T3 conversion impairment rather than the reversing of the vicious cycle.
4. There are people who seem to have a greater predisposition towards developing Wilson’s Temperature Syndrome. Their presentations of the symptoms of Wilson’s Temperature Syndrome are generally less dramatically associated with precipitating events. They more often have had the symptoms for many, many years, possibly for their entire lives. So it is more difficult for them to be able to notice the onset of the symptoms since they don’t really know what it feels like to be “normal.”
5. When patients are asked about their past medical history, it is often found that they have been treated with many of the symptomatic treatments that are listed later in this chapter. They may even have been diagnosed as having a “thyroid” problem and told that they need to stay on thyroid medicine “for the rest of their lives.” If DTSF goes widely misunderstood, and is commonly overlooked today, then certainly it has been misunderstood and overlooked previously, and thus, not all past thyroid diagnoses are necessarily correct. Patients who have been told they have a “goiter” may not have had a “goiter” (swelling of the thyroid gland due to stimulation of the thyroid gland by TSH, thyroid stimulating hormone). Patients may have been told that they had frank hypothyroidism when they did not. Especially considering the difficulty in actually measuring the thyroid hormone/thyroid hormone receptor interaction. All previous thyroid system diagnoses should be taken with a grain of salt. Because, even if the diagnoses are correct, they may not be the only thyroid system abnormality present causing the symptoms of DTSF (there are several causes of DTSF and more than one can be present at one time). There have been patients that I have treated who were diagnosed as having hypothyroidism twenty years ago. They were started on T4 medication and told that they were going to remain on T4 for the rest of their lives. Yet, even with T4 medication the patients’ symptoms of DTSF remained inadequately addressed. With the WT3 protocol the patients’ symptoms were relieved with the symptoms remaining persistently better even after all thyroid hormone medication had been gradually weaned. Patients diagnosed in the past as having hypothyroidism may actually have had Wilson’s Temperature Syndrome. If the patient states that his “hypothyroidism” happened twenty years ago after he was involved in a major car accident or divorce, then the likelihood the patient actually had Wilson’s Temperature Syndrome increases. This is because Wilson’s Temperature Syndrome is more commonly brought on by a precipitating event or major life crisis than is hypothyroidism. 6. Of course, when a patient is taking thyroid hormone therapy, their own thyroid system function is suppressed temporarily. It is interesting to see patients’ thyroid glands come up and function normally even after they have been suppressed for twenty or thirty years. These patients may never have suffered from hypothyroidism in the first place, but rather from Wilson’s Temperature Syndrome.
It is hard to imagine that such a simple problem can cause so many and such severe complaints and can stay in a person’s body for so long when it frequently can be corrected so quickly and easily with proper treatment. It can be a very touching thing, because many patients that I see, when their symptoms resolve quickly with treatment, are often tearful when they realize that they don’t have to spend the rest of their lives feeling unwell. It’s sad when they realize that twenty or thirty years of their lives have passed, and once thirty years have passed. Those years can’t be retrieved or relived. Although the burden may be lifted for the rest of their lives, it is sometimes bittersweet, because they sometimes can’t help but look back and wonder how things might have been if the problem had been treated thirty years earlier.
Maladaptively Slow
Somewhere along the line a person decides when their complaints and conditions are normal and when they are abnormal. Doctors also make the distinction between normal or abnormal as they are deciding whether or not to treat a particular condition. The patients that I treat usually determine their complaints to be abnormal when they feel they are inappropriate under the circumstances. It is normal to feel bad when one is sick with a cold, sore throat or other ailment. And when one has lots of pressures and stresses, it is understandable when one doesn’t feel on top of the world. People recognize they have a problem, however, when their feelings cease to be appropriate with the things that face them. Different patients may express this in different ways:
“I get plenty of sleep and I’m still tired.”
“I can’t understand why I am depressed and having these bad feelings because there is nothing that’s going wrong in my life, everything is fine.”
“I can’t understand why I can’t concentrate and why I can’t remember things.”
‘I can’t understand why I can’t get anything done at work when I used to be extremely sharp, and my business isn’t really that challenging right now.”
“My business is not extremely difficult, but I’m still having trouble functioning and trouble accomplishing even the smallest things.”
“I can’t understand why I’m so irritable, mean, and abusive towards the people that I love the most, namely; my family, my spouse, and my children.”
“It literally scares me to look at my child, who I love more than anything else, when five minutes earlier I exploded in a rage of temper towards him for no good reason.”
“I am trying to understand how and why I could possibly have those feelings of anger, considering how much I love my children and my family.”
“I can’t understand why I’m so miserable and depressed because I really love my job.”
“I can’t understand why I’m so anxious, fearful, and overwhelmed now, because everything is fine.”
“I can’t understand why I can’t get things accomplished. I know a sinkful of dishes is not a big deal. I know emptying the garbage is not a big deal. I know that going to the grocery store is not a big deal. That’s why I can’t understand why I cannot get enough motivation, ambition, resources, or whatever it takes, to get it done.”
“I can’t accomplish the smallest things. And I can’t figure it out because I should have plenty of resources to do them. I used to be able to accomplish tasks with no problem, but now I can’t.”
These are typical concerns of Wilson’s Temperature Syndrome sufferers. It apparently is not too difficult for doctors to determine when a patient’s symptoms seem to be inappropriate because they frequently treat the symptoms of Wilson’s Temperature Syndrome separately, which will be discussed later in chapter 8.
Low Body Temperature
Wilson’s Temperature Syndrome is characterized by a body temperature that runs, on average, below normal. Dr. Barnes’ temperature test involved taking an underarm temperature using a glass thermometer as soon as one awakens in the morning (before rising).
For optimal enzyme function, it is important that the body temperature patterns run neither too high, too low, nor too unsteady. It is well known that the body temperatures do vary at different times in different situations. For example, body temperature tends to run lower in the morning, rises as the day progresses, and decreases again towards evening on a daily basis. Temperature patterns are also seen to change with monthly menstrual cycles, and it is for this reason that women take their temperature while they are attempting to get pregnant to determine ovulation. I believe there can also be seasonal variations in body temperature similar to the hibernation response in animals. And, of course, the body temperature patterns can be affected by activity, diet, and other factors.
Since the body temperature often follows a daily cycle, I prefer to have my patients take their temperatures orally beginning three hours after they have awakened and every three hours thereafter, three times a day (for example, if they awake at 7am; then take temps at 10am-1pm-4pm). There are several reasons for this:
l. It is understandable that people’s body temperatures may be low upon rising each morning after having been asleep all night, considering the body temperature does tend to be a little bit lower during sleep. But if the body temperature patterns run significantly below normal even during the bulk of the day when they are supposed to be at their highest, then it is more likely that the patient has abnormally low body temperature patterns (thus there may be fewer false positives with this test as compared to the morning temperature test).
2. Since body temperature pattern stability is also important and since body temperatures can fluctuate up and down within hours, I prefer three readings each day which can help one get an idea of the steadiness of the body temperature pattern as well as how high or low the average temperature is. Ideally, the body temperature should be at the proper level and also be steady. If using digital thermometers, patients should make sure to replace the batteries as needed (once every two weeks?), and to not drop their thermometers from higher than 4 inches, otherwise they may become inaccurate. Environmental legislation is making mercury/glass thermometers less available. The important thing is to see the change in the patients’ temps with treatment.
3. Oral temperatures are faster, and more convenient to take during the day than underarm temperatures.
From my experience, I would consider body temperature patterns that vary two or three tenths of a degree when measured several times during the waking hours to be relatively steady. I would consider body temperature patterns that fluctuate an entire degree or more to be relatively unsteady. This degree of unsteadiness, itself, is enough to explain adverse symptoms. I have seen patients that are not on any medicine, have their body temperature patterns fluctuate as much as two and even three degrees during the day.
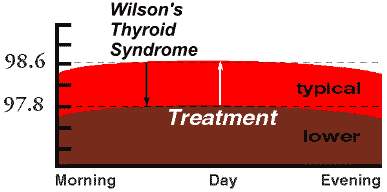
Most commonly, the patients that I see who have symptoms of decreased thyroid system function, typically have body temperatures to average around 97.8 degrees. Some patients can be symptomatic with body temperatures of 98.2 degrees, on average. It is rare, but there are a few people who are symptomatic with body temperatures averaging 98.4 whose symptoms resolve when their body temperatures normalize to 98.6 degrees with the WT3 protocol. Again, most Wilson’s Temperature Syndrome patients’ temperatures average around 97.8 degrees, but frequently patients’ temperatures may be found to average from the high 96’s to the mid-97’s. Sometimes there are patients who are found to have body temperatures averaging in the 95’s. I have seen at least one patient with temperatures in the 93’s. So, although there can be some variation in the body temperature patterns, patients with Wilson’s Temperature Syndrome who are complaining of the symptoms MED generally have body temperatures that average about 8/10 of a degree below the accepted normal of 98.6 degrees. When they receive the WT3 protocol, normalizing their average body temperature to 98.6 degrees, their symptoms are most likely to resolve.
No, not everyone that has a body temperature that averages below normal has DTSF, Wilson’s Temperature Syndrome, or MED. But a body temperature pattern that averages consistently below normal is more than enough to explain the complaints and symptoms of MED, and Wilson’s Temperature Syndrome should be one of, if not the first, possible causes considered. Of all the characteristics of Wilson’s Temperature Syndrome, body temperature patterns have by far the most predictive value in terms of diagnosis and monitoring of treatment. In fact, if a patient’s body temperature pattern does not average below normal, then it is far less likely that he will respond favorably to T3 treatment.