Let’s talk about how the thyroid system affects the body temperature and the metabolism. My patients and I are continually amazed at the effects proper T3 therapy can have in the treatment of Wilson’s Temperature Syndrome. I’m often asked, “How can this one medicine make such a big difference and how can it affect so many things?” It is not hard to understand the far-reaching and pervasive effects of liothyronine (T3) when we remember its critical role in controlling the metabolism – the sum of all chemical reactions in the body. To understand this critical role, let us look more closely at the thyroid system. The following diagram (diagram 2-2) will be referred to as we discuss more fully the thyroid system.
Briefly, the thyroid system begins in the brain. At the bottom of the brain is the hypothalamus, which is the part of the brain that secretes TRH (Thyrotropin Releasing Hormone). TRH travels to the pituitary gland at the base of the brain and stimulates the pituitary gland to produce TSH (thyroid stimulating hormone). TSH enters the bloodstream, travels to the thyroid gland at the base of the neck and stimulates it to produce T4 (thyroxin). The T4 produced in the thyroid gland is
then converted to the physiologically active thyroid hormone T3 (liothyronine). T4 is converted to T3 by an enzyme called 5′-deiodinase, which is found in many of, if not all, the tissues of the body. By far, most of the T3 of the body is produced from the conversion of T4 to T3 that takes place outside the thyroid gland in the body’s tissues. T3 has its action at the nuclear membrane receptors in the cells of the body. There, the T3 initiates a cascade of chemical reactions within each cell and thereby affects each cell’s metabolic rate. The metabolic rate of the cells determines the metabolic rate of the body. The metabolic rate of the body, together with the surface area, activity level, sweating, environmental conditions, and other factors, determines the body’s temperature. The body’s temperature affects the function of the enzymes which are largely responsible for the most important chemical reactions in the body. These chemical reactions, in turn, are the key to the body’s functions. This is the reason that the thyroid system is so vitally important. It affects every bodily function. Indeed, a complete absence of the thyroid system’s function is not compatible with life.
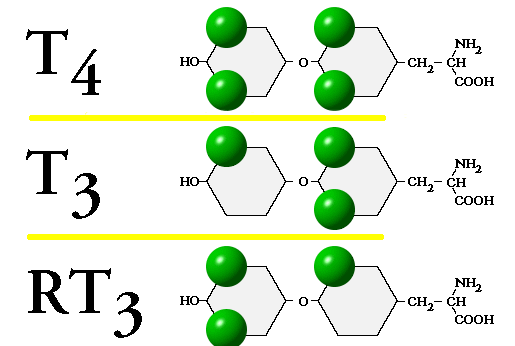
It should be pointed out here that not only can T4 be converted to T3, but also it can be converted to Reverse T3 (RT3). T4, RT3, and T3 look very similar as is demonstrated in the diagram below.
They are like three keys that look the same with each key having one notch that’s different. All three keys may fit into the lock, but they might not work the same. In the same way, T4, RT3, and T3 each have greatly different capacities to stimulate the thyroid hormone receptor. T4 has a small amount of activity at the site; T3 is four times more active than T4; and RT3 has no activity at all. Since T4 and RT3 look so similar, they both can occupy the active site of the 5′-deiodinase enzyme, thereby competing for the enzyme’s attention. It should be noted that stress, fasting, illness, cortisol, and some medicines can also inhibit the action of 5′-deiodinase.
The Inertia Of The Thyroid System
Inertia is the tendency of a body to resist change in its motion. It is the tendency of a body in motion to stay in motion unless acted on by an outside force.
I have paid close attention to the thyroid system (especially the relative levels of T4, T3, and RT3) while treating thousands of patients. Through these observations I have come to believe that the relative conversion of T4 to T3 and RT3, the competition of RT3 and T4 for the deiodinating enzyme, and the relative effect of RT3, T4, and T3 on the nuclear membrane receptors, provide the thyroid system with a great deal of inertia. This means that once the thyroid system is set in a certain pattern, there is a great tendency for it to remain in that pattern. I believe that it is designed this way for a very special purpose.
It would be difficult, within the limits of this book, to convey all the experiences that have led me to this conclusion. But maybe it will help to point out a few observations. Let’s remember that T3 is four times more potent than T4, that it is the most active thyroid hormone, and that it has a half-life of 2 1/2 days. (The half-life of a hormone is the amount of time required for 50% of the hormone present at any given time to be eliminated by the body). Let’s remember that T4 is less potent than T3, and has a much longer half-life (7 1/2 days), and therefore is more “stable” than T3. And RT3 (Reverse T3) has no activity at all and is rapidly broken down by the body soon after it is produced.
Let’s refer to diagram 2-2. Since stress can decrease the amount of T4 converted to T3 by inhibiting the deiodinating enzyme, which causes more T4 to be shunted towards RT3, and since T3 is extremely active and RT3 is completely inactive, it is easy to see how stress can decrease the amount of active thyroid hormone available to the cells.
When the stress passes, there is less direct inhibition of the deiodinating enzyme, which encourages greater T4 to T3 conversion. And there should be less shunting of T4 to RT3, which should result in more T3 being produced. With RT3 being quickly broken down, there should also be less indirect inhibition of the enzyme from competition between T4 and RT3 for the activity of the deiodinating enzyme. These changes should allow the T4 to T3 conversion to return back to normal. Our systems are designed this way to allow the body to slow down under conditions of stress, and then return back to normal when the stress has passed.
Remembering that T4 is a longer-acting and less-potent stimulator, you can see how it can have a stabilizing influence. If T4 had no effect, then the unmitigated influence of T3 at the nuclear membrane receptor might cause a system that lacks sufficient stability. However, since T3 is the physiologically active thyroid hormone, if it did not have its effect, then the much weaker influence of the T4 would almost certainly be insufficient to provide for an adequate level of metabolism. So, we see the beautiful balance of how T3 can provide sufficient levels of metabolism, and T4 can help provide the desired stability. Another factor to remember is that when T4 is broken down, a portion of it is converted to T3. So T4 also serves as a steady, constant supply of the more active T3.
Even RT3, although it is short-lived, seems to play a role as a recent article in a Japanese medical journal suggests. It states that RT3 may play a biologically causative role in decreased thyroid system function. (Nippon Geka Gakkai Zasshi; Shigematsu, H.; October, 1988, 1989; pp. 1587-93). Reverse T3 may play this role by interfering with the T3 / thyroid hormone receptor interaction and/or by competitively inhibiting the deiodinating enzyme. When T4 to T3 conversion is impaired, there is less T3 to stimulate the receptors powerfully, and relatively more T4 to stimulate them weakly. With less T4 to T3 conversion, more T4 may be shunted to RT3, which results in more competitive inhibition of the deiodinating enzyme. This may result in even less T4 to T3 conversion, more shunting towards RT3, and so on. And so a vicious cycle can be started that can contribute to a persistent T4 to T3 conversion impairment that can remain even after the original cause of the impairment has passed. Such a cycle could last for years, and could get worse in stages with subsequent stresses.
An analogy comes to mind that may help one to visualize the inertia of the thyroid system. Let’s imagine a small sailboat placed in a flowing stream. The stream is flowing at a constant speed, but there is a fan placed downstream in front of the sailboat that is blowing upstream. As the sailboat floats downstream and comes closer to the fan, the blowing of the fan keeps the boat at a certain distance, and the flowing water keeps the boat from moving further away from the fan.
Now, if the stream flows more slowly, there is less pressure on the boat to remain close, and it moves upstream, further away from the fan until it settles into a new stationary position. This is because the further the boat moves away from the fan, the weaker the fan’s influence, until the influence of the fan and the influence of the stream equalize again.
But when the flow of the stream increases, the sailboat settles into a new stationary position that is closer to the fan as the two forces again reach equilibrium. So, even though the fan is always flowing, and the stream is always flowing, the sailboat has a tendency to settle into a certain position and stay there as long as the influences remain balanced.
The thyroid system behaves similarly, but is more complex. T4 is converted to T3 and also to RT3. RT3 affects the conversion of T4 to T3. Stress can also affect T4 to T3 conversion. In addition, T4 can interact with the nuclear membrane receptor, as can T3 and possibly RT3. So there are at least six or seven influences at work which are constantly moving, but tend to add up in such a way that the thyroid system settles into a certain position and stays there in much the same way that the sailboat finds equilibrium.
The design of the peripheral (outside the thyroid gland) conversion of the thyroid hormones is set up to provide a great deal of inertia. This is no accident. The peripheral conversion design is probably of far greater importance in the regulation of the thyroid system’s ultimate influence on the metabolism, than the glandular feedback mechanisms (involving the thyroid gland, pituitary gland and hypothalamus) that are currently thought to be most important in this regard.
When You Hear “Thyroid,” Think System Not Gland
How people use the word “thyroid” has led to confusion that has contributed to Wilson’s Temperature Syndrome being overlooked.
For some reason, decreased thyroid system function is not commonly suspected when one is considering possible sources of physical ailments in people who are ill. Since it is not often considered as a problem, it is not commonly talked about or discussed. When the topic is brought up, people will often be heard saying that “so-and-so” has/had a “low thyroid problem.” Most often, people (even doctors) will automatically tend to think of the word “thyroid” as being used as a noun in this context to refer to the thyroid gland. This tendency is reinforced if the first statement generates the question “What’s thyroid?” One would often tend to answer, “The thyroid is a very important small butterfly shaped gland at the base of the neck that …” and so on. This tendency draws attention away from the fact that the thyroid gland is only one part of the whole thyroid system and not even the part with which there’s most commonly a problem. As odd as it may seem, I feel that it may be this simple tendency that has caused Wilson’s Temperature Syndrome to be overlooked by some of the best doctors in the world for decades (by so many for so long). For this reason I recommend that in the phrase “low thyroid problem” the word “thyroid” would best be thought of as an adjective used to describe the entire thyroid system. This would help us all to remember that the thyroid gland is again merely a part.
Which link in bicycle chain is the most important? Without any one of the links, the chain could not perform its function. Would the link that most often breaks deserve the most attention? I recommend in order to keep the proper perspective that we use instead of the phrase “low thyroid problem,” the phrase “decreased thyroid system function” or DTSF. Using this phrase may help us (lay people and doctors alike) from getting too fixated on the gland only. Because when we do this, then we are often led down the wrong path while overlooking some very obvious problems. All the causes of decreased thyroid system function (DTSF) all generate the same symptoms of Multiple Enzyme Dysfunction (MED) that result from body temperature patterns that are too low, but not all causes of DTSF involve the thyroid gland itself.
Let’s discuss the impairments that have been described to date. Rarely mentioned is the possibility of the hypothalamus not producing TRH as it should. This may be referred to as secondary hypopituitarism since it results in low (hypo) function of the pituitary gland secondary to inadequate TRH stimulation. Hypopituitarism can be primary (as in primary hypopituitarism) meaning that the problem is primarily in the pituitary gland itself which results in inadequate TSH secretion. Inadequate TSH secretion leads to hypothyroidism secondary to a pituitary problem (and so primary hypopituitarism is also sometimes referred to as secondary hypothyroidism).
Are we confused yet? The problem may be primarily in the thyroid gland itself which results in inadequate T4 production in spite of normal TSH production (this is known as primary hypothyroidism). The impairments of the thyroid system listed above have been fairly well described to date. However, one may see from the diagram (diagram 2-2) that there is still a long way from the thyroid gland to generation of an adequate body temperature. Impairments of this important portion of the thyroid system have thus far not been well described. One may see from the diagram that there could be a problem with the conversion of T4 to T3. It is known that the conversion of T4 to T3 decreases under periods of fasting and severe illness. It has been shown under these conditions that the level of T4 to T3 conversion can drop by 50%. This change has also been shown to return to normal once the fasting or severe illness is over. When the conversion of T4 to T3 decreases, more T4 is shunted to RT3 causing an elevation in RT3.
These adaptive changes in laboratory findings are not considered to be very serious and are sometimes referred to as “Euthyroid Sick Syndrome.” Although this syndrome has not been very well defined, it is usually thought of as an adaptive temporary change in laboratory tests
This condition has, up until now, not been named or well described. I have taken the liberty to name it Wilson’s Temperature Syndrome and to describe it in great detail in this book. As it turns out, Wilson’s Temperature Syndrome can have a tremendous impact on a person’s life causing characteristic and often debilitating symptoms and being quite maladaptive. It can be brought on by fasting, illness, and stress but rather than going away after the conditions have passed, it can persist; thyroid blood tests are often within “normal range,” but it is characterized by a low body temperature; it can be treated with proper therapy (with the WT3 protocol being very important). With the WT3 protocol the syndrome can be reversed usually with the correction persisting after treatment has been discontinued (although subsequent stress can cause the syndrome to return again).
The symptoms of Wilson’s Temperature Syndrome are essentially the same as the symptoms of other causes of decreased thyroid system function; yet proper treatment of Wilson’s Temperature Syndrome has revealed other related symptoms that up until now have not been very much considered to be thyroid (adjective) related (e.g. migraines, PMS, panic attacks, night sweats, ringing of the ears, mood swings, itchiness, allergies, asthma, etc.).
Of all of the causes of DTSF mentioned above, Wilson’s Temperature Syndrome is by far the most common. As previously discussed, the symptoms of MED can result from low body temperature patterns of various causes. However, DTSF is by far the most common cause of the low body temperature patterns that cause persistent symptoms of MED. And although there are various causes of DTSF, Wilson’s Temperature Syndrome derives its importance from the fact that it is by far the most common of those. It is at least 50 times more common than any other cause of DTSF and therefore is also the most important.