|
Workup
|
Since the patients have already filled out a symptom sheet before I see them, I usually begin with the patient’s past medical history so that I can more easily put the symptoms and chief complaint in context when we discuss them. This cuts down on the amount of “back tracking” and decreases the chances of important points being missed.
The past medical history should include the usual questions about past acute and chronic illnesses, present illnesses if any, surgeries, accidents, and especially the maternity history. Since childbirth is the number one cause of Wilson’s Temperature Syndrome, it is important to take a careful history regarding miscarriages, abortions, ectopic pregnancies, infertility, and full term pregnancies.
It is important to evaluate the patient’s current medicines to see if any are no longer necessary, and to consider possible interactions.
The family history should include stroke and cardiac problems, especially myocardial infarction, cardiac bypass operations, and at what ages these events transpired in the lives of family members. The family history should also include family members given “thyroid” diagnoses.
Next it is helpful to review the patient’s presenting symptoms and chief complaint.
Note: It is helpful to determine from the patients which complaint is bothering them the most. I will frequently ask, “I know all these symptoms can be related, but if we could fix just one thing, what would it be? Which of them is bothering you the most?” It is sometimes difficult for patients to narrow it down to just one, but they can almost always narrow it down to two or perhaps three symptoms.
When the chief complaint has been determined, it is useful to carefully characterize the presentation of the symptoms, as the presentation can be very predictive.
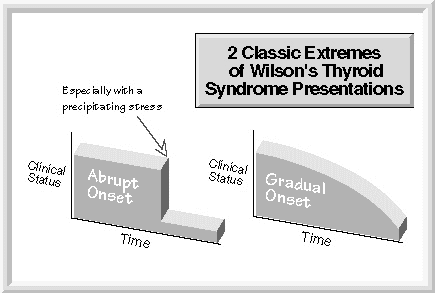
There is a continuum of presentations with two classic presentations at either end.
One presentation (abrupt onset) is typical of those people who are constitutionally resistant to developing Wilson’s Temperature Syndrome, but who do because of overriding circumstances.
The other presentation (gradual onset) is typical of those people who seem to have a constitutional predisposition for Wilson’s Temperature Syndrome.
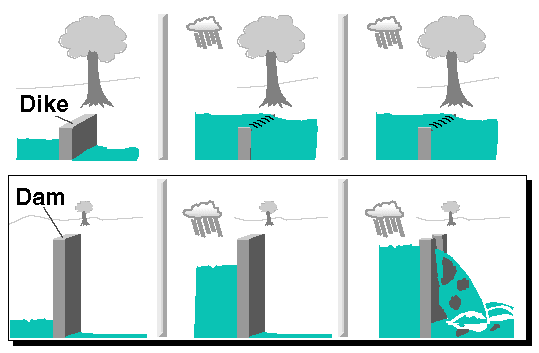
I like to use an analogy to illustrate the differences. A small dike provides a little resistance to the flow of water. A large dam provides a great deal more resistance.
When heavy rains upstream send water downstream that challenges the dike, the water builds up behind it and soon begins to overrun it. And as the problem becomes worse and worse the “dry” side becomes more and more wet, so there is a gradual transition from dry to wet.
On the other hand, when heavy rains upstream challenge the dam, the water builds up behind the dam with great pressure; but on the dry side of the dam, little change is observed. However, if that dam were to receive a challenge too great, and finally give way, there would be a horrendous amount of change taking place very quickly, so there would be a very dramatic transition from dry to wet.
Likewise, the symptoms of patients who have less resistance to developing Wilson’s Temperature Syndrome typically come on more gradually out of the blue without as clear-cut a precipitating stress. On the other hand, patients with more sturdy metabolisms, that are less predisposed to developing Wilson’s Temperature Syndrome, typically have their symptoms come on more dramatically in a group after a more identifiable precipitating stress.
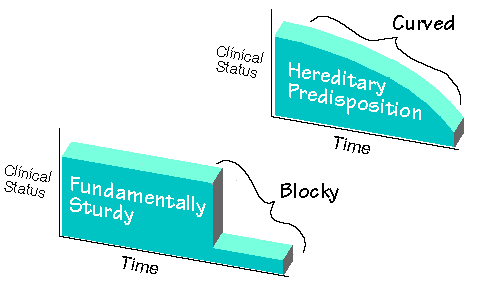
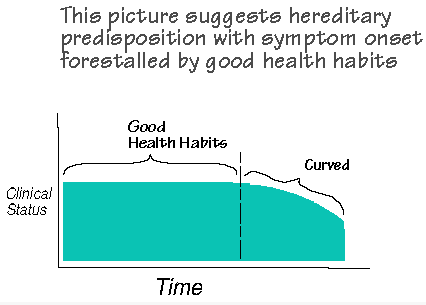
Those with hereditary predispositions for Wilson’s Temperature Syndrome typically have a more curved picture of onset. Those patients with more fundamentally sturdy metabolisms tend to have more blocky pictures of clinical onset of Wilson’s Temperature Syndrome.
As soon as the patient begins to give me a curved picture upon questioning, I begin to think hereditary predisposition.
As soon as I get a blocky picture, I think of a fundamentally sturdy metabolism.
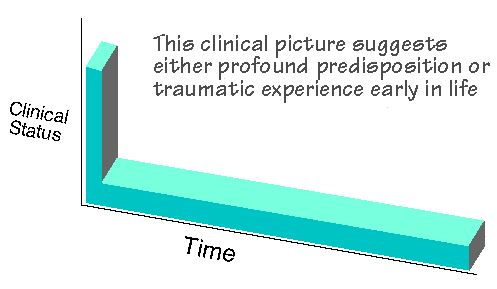
There are some mixed pictures, however, as seen below…
A traumatic esperience early in life (such as abuse), can bring on Wilson’s Temperature Syndrome abruptly, early in life.
What if a patient goes down in one fell swoop early in youth? It suggests that either the patient has a profound predisposition for a slowing of the metabolism, or it suggests that something very traumatic happened then in the life of that patient.
This traumatic event may frequently be abuse of one type or another. Sometimes this provides an opportunity for the patient to discuss traumatic experiences they have never before divulged to anyone.
A traumatic esperience early in life (such as abuse), can bring on Wilson’s Temperature Syndrome abruptly, early in life.
What if a patient goes down in one fell swoop early in youth? It suggests that either the patient has a profound predisposition for a slowing of the metabolism, or it suggests that something very traumatic happened then in the life of that patient.
This traumatic event may frequently be abuse of one type or another. Sometimes this provides an opportunity for the patient to discuss traumatic experiences they have never before divulged to anyone.
If a patient’s symptoms come on more gradually, more management may be needed to correct the problem.
Note: Above, and on the following pages are 6 questions that more fully characterize a patient’s presentation. It is my contention that if one asks 100 patients treated with T3 these questions prior to treatment, then one will gain 100 patients worth of experience. If one does not ask these questions one will not gain 100 patients worth of experience (that is, experience useful in helping one predict before treatment how a patient’s course of treatment is likely to go). This is because the parameters ascertained by the questions are the ones I have found to be the most predictive.
When symptoms come on together it is more likely they are relaxed.
As indicated earlier, when the symptoms come on more gradually, it suggests the person is more predisposed to a slowing of the metabolism.
Generally speaking, the more abruptly the symptoms come on, the less management is needed to correct them. Also, such a person is less likely to relapse once treatment is discontinued than is someone more prone to a slowing of the metabolism.
In general, when patients report that their symptoms have come on in one stage, their symptoms are generally easier to correct, perhaps with one cycle of T3 therapy (especially if the symptoms are not very long-standing).
When a person’s symptoms worsened in stages, it suggests the patient is a few more steps out-of-bounds, and more cycles of T3 therapy may be necessary to correct the symptoms.
A pretty good rule of thumb is that the number of cycles that may be needed to correct the problem is generally commensurate with the number of stages in which it developed.
Suppose a patient says: “I was fine until about 10 years ago when I developed these symptoms after a bankruptcy; the symptoms stayed about the same until they worsened about 5 years later when I divorced; the symptoms then stayed about that bad until a year ago when my mother had a heart attack, and was expected to die.” This is three stages down, and may very likely require 3 cycles to bring back up.
Patient’s with more mild presentations often respond more quickly and easily.
The longer a patient has had the symptoms, generally the longer (and perhaps more cycles) it takes to correct them.
Patients requiring more cycles of T3 therapy also tend to need higher doses, at least initially.
If patients have only had the symptoms for 6 months, their Wilson’s Temperature Syndrome can frequently be corrected with one cycle on relatively low doses of the medicine, in about 3 -6 weeks. In other words they can frequently be snapped back into place fairly easily.
Don’t be afraid to consider T3 therapy in a patient who has a more mild presentation, since they usually tolerate it easily, and respond the best. It is often better to “nip it in the bud” rather than let the problem become worse and more difficult to manage.
Note: Interestingly, age, sex, and weight are not very predictive in terms of dosage levels that may be needed.
People of certain nationalities are more predisposed to developing Wilson’s Temperature Syndrome, and are generally more difficult to correct, and more prone to relapse.
To review, it seems that those who are most prone to developing Wilson’s Temperature Syndrome are those whose ancestors survived famine, such as: Irish, American Indian, Russian, Scot, Welsh, etc.. The combination that seems most predisposed are those persons who are part Irish and part American Indian. And the symptoms of patients who are more predisposed tend to come on more gradually.
Such patients are a little more difficult to correct, especially if their symptoms are long-standing.
They are more likely to relapse with less provocation.
They frequently have reddish highlights in their hair, and a fair complexion with some freckles.

It is a relatively good sign if thyroid treatment has helped for any period of time in the past, because then it is more likely that they will be responsive to T3 therapy.
As discussed previously, it is a relatively bad sign if a person relates a story consistent with being pushed too far in the wrong direction with the wrong (T4-containing) medicine.
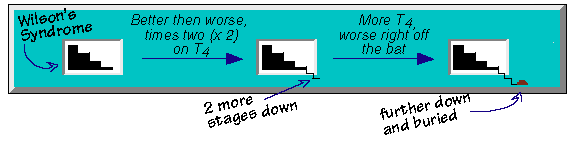
When Wilson’s Temperature Syndrome patients get better with a T4-containing medicine and then get worse again, their conditions have gone one more stage in the wrong direction. And if they get worse right off the bat with a subsequent increase in the T4-containing medicine, it’s as if they have been pushed even further out-of-bounds and buried there.
They can be uncovered and brought back in bounds, but it will frequently take more cycles (these patients are typically the hardest of all to to correct).
It is suggestive (and not uncommon) if a patient’s symptoms come on and persist after a cortisone shot, or a liquid diet, because these can both strongly inhibit T4 to T3 conversion.
Of course, medical treatments that can involve a great deal of stress can also be associated with the onset of Wilson’s Temperature Syndrome. For example, chemotherapy for cancer, abortion, mastectomy, and many other medical problems and surgeries.
It should be pointed out that even hypothyroid patients who are well-managed on T4-containing medicines can develop Wilson’s Temperature Syndrome just like anyone else.
For example, another common scenario is the euthyroid patient who becomes hyperthyroid, and has her gland ablated surgically or with radiation. She then requires T4 supplementation, but develops and continues to suffer from symptoms of hypothyroidism, in the face of normal blood tests. This is not good, it is not normal, and it is not “to be expected, and to be learned to live with.” The patient did not have hypothyroid symptoms before hyperthyroidism, and shouldn’t have them after hyperthyroidism. The shock of the illness and it’s treatment can push such a patient into Wilson’s Temperature Syndrome. This is frequently easily managed by cycling the patient with proper T3 therapy (supporting between cycles with T4), and getting the patient to be much more clinically euthyroid, on less T4-containing medicine than she had been taking.
|
Some signs of decreased thyroid system function
|
The physical exam should look for signs of decreased thyroid hormone system function (dry skin, dry hair, fluid retention, thinning of the lateral third of the eyebrows, thinning of the hair of the body and head, periorbital edema, and others).
Part of the workup includes having the patient record her body temperature patterns in a temperature log to document that they run below normal on average.
The thyroid gland should be examined for any nodules, goiter, or tenderness.
The patient’s skin may appear to be more dry, coarse, and wrinkled than might otherwise be expected.
She may have a little bit of puffiness in her face, especially around her eyes. The puffiness is often extremely subtle and can sometimes only really be imagined after having seen many cases of Wilson’s Temperature Syndrome before and after T3 therapy. If more severe, the mild puffiness around her eyes might even be reminiscent of someone who has just woken up.
Before therapy the patient’s facial features may appear to be slightly “fuller.” After therapy they may appear “sharper,” almost as if the patient’s appearance and features become more “focused.”
The patient may have artificial nails or peeling, splitting nails that break easily or that are soft. It may be possible to see her scalp through her hair.
With some experience treating Wilson’s Temperature Syndrome, you’ll be able to walk through a shopping mall and identify people that are likely to have low body temperatures.
|
Tests
|
Tests are done to evaluate the patient’s thyroid hormone system status, risk of T3 therapy, and to rule out other possible explanations for the patient’s symptoms as well as conditions that can be made worse. They should include a baseline EKG.
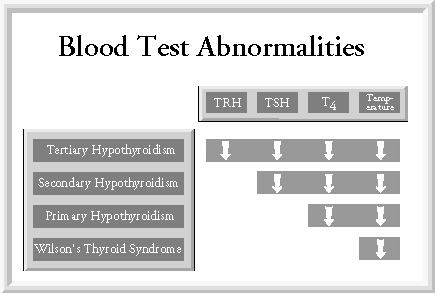
Tests can include T4, TSH, total T3, total RT3, multichemistry, complete blood count, EKG, ANA, and others.
Special care should be taken to rule out as well as possible, conditions that can be made worse with thyroid hormone supplementation (for example, cardiac arrhythmia, Addison’s disease, and others).
I recommend a baseline EKG on all patients.
Note: There are other precedents for “peripheral” hormonal problems that don’t show up on blood tests.
Menstrual cycles are known to be controlled by female hormones. However, irregular periods are not diagnosed by female hormone blood tests. Neither are they treated according to blood tests. Doctors will often treat irregular periods with several months of birth control pills to artificially reestablish normal menstrual cycles that often remain improved even after the pills have been discontinued. Likewise, whereas Type I Diabetes is due to inadequate insulin production by the pancreas, Type II Diabetes is often due to insulin resistance or improper response, for whatever reason, to the insulin produced by the pancreas. Patients with high blood sugars are treated even if their bodies are producing insulin (Type II Diabetes).
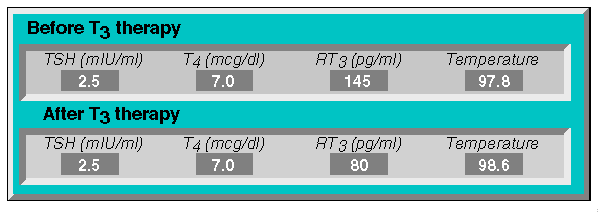
Likewise, patients with low temperatures and hypothyroid symptoms can be treated even if their bodies are producing T3 (with T4 and T3 levels being within normal range on blood tests).
If the unfavorable conditions progress, a person could develop an arrhythmia, most commonly atrial fibrillation.
In such cases, the baseline EKG might appear to be normal sinus rhythm at first glance, but with careful scrutiny with a pair of calipers, vestiges of irregular irregularities might be detected.
It is good to review the baseline EKG carefully for such abnormalities, since their discovery allows one to advise a prospective candidate for T3 therapy that they may be more likely to develop such manifestations.
Such findings on the presenting EKG are not an absolute contraindication to T3 therapy, but serve to let one know what to watch out for. These kinds of manifestations can be avoided by watching carefully for any such signs, and then adjusting the treatment at the first sign of such problems to see to it that they resolve (this can include weaning completely off the T3 therapy).
Special care should be taken in elderly patients. And there are many patients who would not be good candidates for T3 therapy at all, because of their cardiac or cerebrovascular risk.
For example, one can see some interesting things happen to RT3 levels in a given patient: