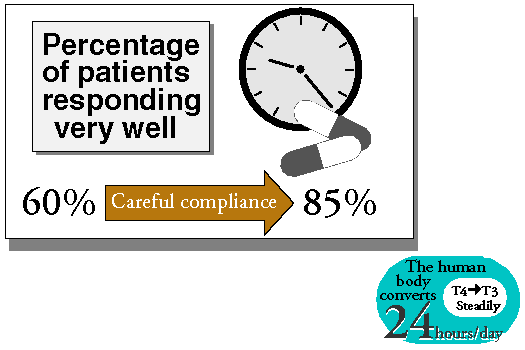
How well on time the T3 doses are taken is very important to the overall steadiness of the T3 levels.
If 100 patients were on T3 therapy and were missing their doses by 15 minutes here, and 20 minutes there, about 60% of them would be responding pretty well to the treatment. However, if those 100 patients took their T3 doses very much on time (within a few minutes of the dose time), then about 85% would be responding very well to the treatment.
It is surprising how much of a difference it makes to take the medicine very much on time, until one considers the physiology involved.
The body makes T3 (from available T4), a little at a time, around the clock, 24 hours a day. So ideally, it would be best if the T3 taken by mouth could also be delivered a little at a time, around the clock, 24 hours a day.
I believe that T3 compounded with a sustained release agent like that used in many sustained-release medications on the market, does a much better job at approaching this than does traditional, or instant-release T3 therapy (e.g. Cytomel).
The sustain-release technology available now is very good but it is not perfect. But nevertheless, very satisfactory results can be obtained if the T3 compound (designed to be taken every 12 hours), is taken as well on time as it can be taken-not even 3 minutes late.

If patients miss the dose by an hour, more than likely they will not notice any difference at first in the way they feel. And so they might assume therefore that it doesn’t really matter very much how they take the medicine. But if the patient misses the dose by 10 minutes here, and 20 minutes there, that can add up over a period of a week or two and the therapy may not work as well.
When patients marvel at my requesting them to take the medicine so well on time, I often joke that it saves them from dragging an I.V. pole around behind them all day long. And this I do to help them picture what we are trying to accomplish. It is easy to see what a difference it makes when patients take the T3 therapy very much on time.
It is true that about 6% of patients seem to do better when they don’t take their doses so much on time, or when they use Cytomel instead of the T3 compound I recommend (p112), but by far most patients do better when they are taking the T3 compound very much on time.
Note: I often ask new patients what is the latest time they wake up on the weekends. If they wake up at 9am on the weekends, and 7am on the weekdays, they might consider taking the medicine at 9am and 9pm every day, so that they don’t have to wake up at 7am on the weekends. Alternately, they may take the medicine at 7am and 7pm everyday if that is easier, but they will then have to set a 7am alarm on the weekends (they can go back to sleep if they like). Of course, “weekends” here represents the days the patient usually gets up the latest, which may or may not be Saturday or Sunday.
The lower the dose the easier it is to keep steady, so it’s best not to use more than is needed. It’s also liothyronine not to go off the T3 all at once (unless on the smallest dose), but to make smooth, gradual transitions.
It’s best to start low and then to increase the T3 dose gradually, in order to use the smallest effective dose. The lower the exogenous dose, the easier it is to keep the T3 level steady. If one uses a large starting dose, or increases the dose in large increments, one may overshoot the lowest effective dose, thereby waiving progress and benefits by using an unnecessarily high dose.
It’s like using a ladder. It’s good to start on the bottom rung and to go up one step at a time, not going higher than is necessary or preferable.
When at the top of the ladder, it’s also good to step down a rung at a time instead of jumping off all at once (and taking the chance of breaking a leg).
Not only may patients poorly tolerate stopping the medicine abruptly, but doing so can also squander benefits obtained in the cycle by not giving the system enough time to effectively maintain endogenously what may have been re-established artificially.
In addition, stopping the medicine abruptly can also create a disturbance that could take 2 weeks to settle down before one could get a fresh start on the next cycle (if needed). Whereas, if things are let down easy with the cycle being weaned gradually and smoothly so that the endogenous system has enough time to come up steadily, then one should be able to get a relatively fresh start on the next cycle about 2 or 3 days after being completely off the present cycle.
Finally, there is no need to “wean gradually” off the medicine when one is taking the smallest dose. When one is on the bottom rung of a ladder, one simply steps off.
| Compounding is the preparation of a medicine by a pharmacist for an individual patinet according to a physician’s specifications. The practice of compounding predates the mass-production, or manufacturing of drugs. |
There are two classes of pharmaceutical preparations in use today. One is manufactured pharmaceuticals, and the other is compounded pharmaceuticals.
Manufactured pharmaceuticals are mass-produced by drug companies and are therefore regulated by the FDA.
Compounded pharmaceuticals are prepared by pharmacists according to a doctor’s prescription, and the pharmacists are regulated by their state boards of pharmacy.
Primarily because of the interest, labor, and expertise necessary, relatively few pharmacists are interested in specializing in compounding pharmaceuticals.
When a physician feels that it is what would best meet the patient’s needs, he or she can have a medicine tailor-made (compounded) for the patient according to his/her specifications by a compounding pharmacist.
Most commonly, compounded pharmaceuticals are used to help bridge the gap between the interests of pharmaceutical manufacturers and the interests of individual patients. This is often done by providing a compound of a medicine that has been discontinued by a manufacturer for market reasons or otherwise, or by providing a familiar drug in an alternative dosage form for the patient’s sake (e.g. suppository for a person who can’t swallow pills well, or that is vomiting).
Compounding is especially useful in situations when the desired dosage level or form of delivery of a drug is not now, and never has been available on the market from a drug manufacturer.
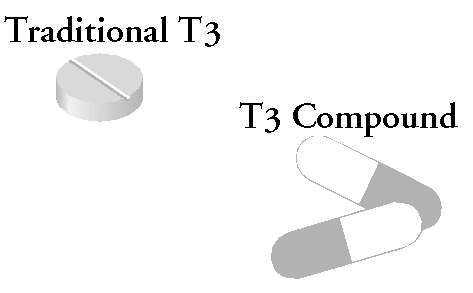
There are two types of T3 preparations. One is traditional liothyronine (e.g., Cytomel ) which is not sustained-release. The other is a T3 preparation compounded to incorporate a sustained-release agent (HPMC) used in many of the sustained-release medications on the market.
At first, I used only traditional T3 (see also p111). I noticed that patients would often get more benefit, with much less chance of side effects if they took the traditional T3 every 3 hours, 6 times a day, instead of only once or twice a day.
It became very apparent that a little medicine taken at intervals, throughout the day, worked much better than a lot of medicine all at once.
A T3 preparation incorporating a sustained-release agent was called for, but no such preparation was available on the market, so I asked a compounding pharmacist to prepare one (the T3 compound) for some of my patients.
The T3 compound utilizes what is known as a hydrophilic matrix system, designed to dissolve slowly to release the active ingredient.
The performance of many products utilizing matrix systems is already well documented (e.g. Dow Chemical Co.), so there is a body of data to reference and rely upon (and HPMC or HydroxyPropylMethylCellulose is often the polymer of choice in matrix systems).
Typically, the higher the concentration of the HPMC in a capsule, the longer it takes the capsule to dissolve. When I first began using the HPMC compound, designed to be taken every 12 hours, the patients reported significantly better results than with traditional T3.
I asked how well and how long the doses seemed to work. Quite a few patients noted that the medicine seemed to begin wearing off about 30 minutes before the next dose. So I asked the pharmacist to increase the preparation’s concentration of HPMC. Then, many reported that it seemed to last until about 15 minutes before the next dose. So the concentration of the HPMC polymer in the capsules was increased again. Many patients reported it seemed to begin wearing off about 5 minutes before the next dose. So the concentration of the HPMC polymer was increased again, until finally, it seemed to last 12 hours based on clinical observation.
This suggests that patients can detect small changes in their T3 levels. It doesn’t suggest that all of the T3 is gone after the dose wears off (since the half-life is 2.5 days), it just suggests that enough of the T3 is gone that the patient can feel the difference (p74).
For best results, one should clinically titrate the preparation one uses (in this manner using a large number of patients), or use one that he or she feels has been. And one should routinely ask patients for these kinds of observations, to see if a pattern emerges.
Note: You may have noticed that I have not called this compound “sustained-release T3.” Officially, a drug is not said to be sustained-release or time-release until blood studies have demonstrated such delivery according to FDA guidelines.
It is clear that with T3 therapy for Wilson’s Temperature Syndrome, steadiness is everything. It has also become clear that the skill, care, and consistency with which the pharmacist makes the compound is crucial (this is even more so the case with T3 than it is for other compounded drugs that incorporate a sustained-release agent), and that the abilities and interests of compounding pharmacists are not all the same, so some care should be taken in selecting one.
| T3 therapy is not a cure-all and is not completely without risk; but if it is implemented as well as it can be, it is generally well-tolerated and often very effective. |
To provide different concentrations of HPMC, fillers such as lactose, talc, starch or kaolin are often employed. Lactose has very nice properties. Capsules that contain lactose may aggravate the infrequent patient with lactose intolerance and another filler may be substituted.
Subjectively, I feel the compounded T3/HPMC preparation is about 20 times more effective in the treatment of Wilson’s Temperature Syndrome, while the incidence and severity of side effects is about 20 times less as compared to traditional T3.
Note: As mentioned earlier, about 6% of patients do seem to do better with traditional T3 as compared to the T3 compound, or with a T3 compound dosing regimen that is less consistent in terms of timing; but by far most patients do better on the T3/HPMC compound taken morning and night exactly on time every 12 hours.
To illustrate the difference, if one were treating 100 patients for Wilson’s Temperature Syndrome with traditional T3 therapy, it would not be surprising for one to receive phone calls from about eight people over a weekend, needing an adjustment in treatment because of rather significant side effects. On the other hand, if one were administering the T3 therapy using the T3/HPMC compound, it would not be unusual for one to go 6 months without receiving an after-hours page.
Proper T3 therapy is a comparatively aggressive/deliberate approach. And if one is going to be aggressive/deliberate with T3 in very many patients, I would not recommend that it be done with traditional T3, but with T3/HPMC compound.
It is usually best for the patients to have a return office visit two weeks after starting the T3 therapy.
I recommend T3 capsules of the following strengths: 3.75, 7.5, 15, 22.5, 30, 37.5, 45, 52.5, 60, 67.5, 75, 82.5, and 90 micrograms (higher doses are sometimes used).
I recommend a starting dose of 7.5 mcg (3.75 mcg may be used in the very rare patient for whom 7.5 is a little too high).
I recommend increasing the T3 dose in 7.5 mcg increments by having the patient go up to the next highest strength each day, as needed.
One reason that it is usually best to use an assortment of capsules of different strengths, is that the cost is much more in the labor of making the capsules than it is in the ingredients they contain. Therefore, taking five 7.5 mcg capsules each dose instead of one 37.5 mcg capsule can be almost 5 times more expensive. Also, the more capsules that are taken each dose, the more gel-forming polymer is introduced into the gut, and some patients have reported diarrhea when larger numbers of capsules are used.
Note: It is usually best for the patient to get a 96-capsule “starter pack” of the medicine, that contains thirty of the 7.5’s and thirty of the 15’s, with twelve each of the following strengths: 22.5, 30, and 37.5mcg.
Since the patient may be changing the dose every day, it is important that she have enough of the medicine to maintain or increase her dose as needed without running out before her next appointment (usually 2 weeks after starting). This minimizes the chances of the patient experiencing a hold-up in her progress in the therapy, or even a set-back. If her progress is disturbed, a couple of weeks of progress can be lost. Not to mention the aggravation and inconvenience to the patient and the office in having to call in another prescription, and having to make adjustments and compromises in her dosing until she gets the prescription; or perhaps even having to make arrangements for the office to give her a few capsules to hold her over.