If a drug does not interact with the T3 a patient’s own body makes, then it will not chemically interact with the T3 therapy she takes by mouth. However, T3 therapy can interact indirectly with other medicines in that all medicines can have side effects, and those side effects can be additive. For example, T3, decongestants, antihistamines, antidepressants, and asthma medicines can lead to nervousness, jitteriness, and palpitations. So when taken together, the chances of those side effects occurring may increase. Likewise, beta-blockers can suppress some of the mechanisms the body uses to adjust to T3 therapy (increased sympathetic tone in response to a drop in blood pressure in a patient who has over-compensated to an increment in dose of T3). Thus, patients whose blood pressure is being controlled with an ACE-inhibitor, or diuretic are more likely to acclimate very easily to T3 therapy.
| (Synergistic) +/- (Antagonistic) |
Also, the body is a complex, interrelated system. And a drug that has its effect on one part of the system can indirectly have an effect on another part. So, the effects of two drugs working on slightly different parts of the system, can have indirect effects that enhance the effects of the other, or diminish them. For example, the direct and indirect effects of the administration of estrogens, progesterones, adrenal hormones and others, may enhance or diminish a patient’s responses to T3 therapy. If progress in T3 therapy seems to be impeded, changes in the dosage of other medicines a patient is taking sometimes frees up the system enough for progress to continue (e.g. decreasing a conjugated estrogen dose from .625mg/day to .3 mg/day).
It is much more important to take the T3 therapy very much on time than for it to be taken on an empty stomach (which might provide a little more consistency in the dosing conditions from dose to dose). For this reason, I do not instruct that the medicine should be taken on an empty stomach because when such counsel is given, patients will frequently miss their dosage times by hours at a time trying to accomplish it.
Interestingly, if a patient changes time zones, then he may experience symptoms of unsteadiness even if his T3 therapy dose stays on the time schedule of his original time zone. My favorite explanation for this phenomenon is the changes in the influence of the adrenal hormone system on body temperature patterns that results from a mild change in diurnal variation as influenced by the stimulation of the retinae by light, and perhaps also because of consequent changes in dietary patterns.
If the patient is not having any complaints with T3 therapy, then he or she may exercise normally. Generally, if the patient was going to have much difficulty while exercising, the patient would likely be able to notice some warnings or symptoms of unsteadiness prior to exercise. It is generally recommended that the patient follow a moderate exercise program to help encourage his/her body to return to normal health.
Alcohol, caffeine, and smoking can influence proper T3 therapy because they can influence body temperature patterns, and it is generally best to avoid these substances during treatment. There is, however, no direct chemical interaction with thyroid hormones and alcohol, caffeine, and smoking. But since the side effects of caffeine, smoking, and alcohol can be similar to the side effects of thyroid hormone therapy, their effects can be additive.
For patients who have inconsistent sleep and work hours (e.g.-changing work shifts every other week) it is sometimes more difficult for them to respond as easily to T3 therapy because of their tendency toward unsteady T3 levels.
The thyroid system is dynamic and not static. If the patient responded in a certain way to a thyroid medicine given a certain way in the past, that does not necessarily mean he or she will respond in the same way if that medicine were to be given again. Also, how a person has responded to medical therapies, stresses, lifestyle changes, diets, and other influences before proper T3 therapy doesn’t necessarily predict how that person will respond to such influences during or after T3 therapy.
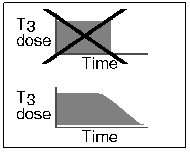
It is not wise to stop the medicine abruptly. If 100 patients stopped their T3 therapy abruptly, about 90% would not have complaints, about 5% would notice significant fatigue and achiness, and about 1% might feel exhausted, lightheaded upon standing, and/or clammy, even to the extent of being rather incapacitated for several days or even a few weeks.
Thyroid medicine is pregnancy category A, which is the safest category for medicines that can be taken during pregnancy. In fact, it can be instrumental in helping a woman to conceive and carry a pregnancy to full-term. Although patients have stayed on T3 during their pregnancies, I usually recommend that patients wean slowly off (one increment every 7 – 10 days) the T3 therapy if they become pregnant while taking it. This is because, if for some reason (e.g., natural disaster) a patient ran out of medicine abruptly and did not have access to more, there would be a small chance she could miscarry. Remember, at the present time many physicians are still not familiar with the principles of management of T3 therapy, so if the patient was involved in a car accident out-of-town, the doctors treating her might not know she was taking T3 therapy, and might not know the significance of proper management (with respect to T3 levels/body temperature pattern considerations) even if they did.
These same concerns would apply to a patient with severe complications during her pregnancy or at the time of delivery. Fortunately, many women with Wilson’s Syndrome feel their best while they are pregnant. Unfortunately, they will frequently go down hill again after the pregnancy, sometimes being worse than they were prior to the pregnancy.
I suspect that Wilson’s Temperature Syndrome sufferers frequently improve during pregnancy because the developing fetus produces human chorionic gonadotrophin (HCG) which can increase the patient’s body temperature patterns and function.
Likewise, I generally recommend that patients wean off T3 therapy before undergoing general anesthesia. This reduces the number of variables with which the physicians involved need to contend. Also, it is good for T3 levels to be steady, and they are more steady when endogenously produced. If the time is short before surgery, and there is insufficient time to wean the T3 therapy normally, then the patient can be supported with exogenous T4 while the T3 is weaned quickly, or stopped abruptly for some reason.
| Therapeutic Symptomatic Prophylactic |
How T3 therapy is managed depends, in part, on what one is trying to accomplish. T3 can be employed as symptomatic, therapeutic, or prophylactic therapy. That is, T3 therapy can be used in an attempt to treat symptoms, to correct symptoms, or to prevent symptomatic relapse. Ideally, we would like to see patients enjoy persistent resolution of their symptoms even after they’ve been weaned off the T3 therapy. But if some other factor is preventing a person from remaining normal when the treatment is discontinued (e.g., stress, lifestyle, or some other hormonal imbalance, or nutritional deficiency), some patients are grateful that they can at least enjoy resolution of their symptoms while they are on the T3 therapy. One patient who was doing well off the T3 therapy noticed that she could prevent small relapses by taking the smallest dosage level of T3 therapy the day before, the day of, and the day after events she knew were going to be stressful.